93% of American Adults are Unhealthy – A Deeper Dive
A recent report (2022 study) claimed that only 6.8% of American adults have optimal metabolic health.
Their analysis comes from data on adults in the United States age 20+ years that is considered to be representative of the nation – the National Health and Nutrition Examination Survey (NHANES) from 1999-2000 to 2017-2018. It’s worth noting that this data precedes the COVID-19 pandemic, which has contributed to a worsening of obesity and presumably other measures, as well.
2019 report on metabolic health
In 2019, we learned (2019 study) that 88% of American adults had at least one feature of the Metabolic Syndrome, per NHANES data as of 2016.
The 2019 study assessed the presence of the 5 criteria for Metabolic Syndrome, along with the absence of taking medication for each criterion:
- abdominal obesity – waist circumference <102/88 cm for men/women
- blood pressure – <120 systolic and 80 diastolic
- fasting blood glucose <100 mg/dL and HgbA1c < 5.7%
- triglycerides < 150 mg/dL
- HDL cholesterol ≥ 40/50 mg/dL in men/women
How do these reports differ?
Let’s examine the difference in criteria utilized in the 2022 study (see figure):
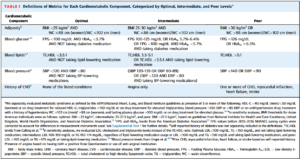
- Adiposity is being defined as both waist circumference within range as well as BMI less than 25 kg/m2. Body Mass Index (BMI) is simply a ratio of one’s weight (in kilograms) to the square of one’s height (in meters), not a reliable measure of adiposity. It’s convenient to use for large groups of data when only basic measurements are known, but it doesn’t reliably reflect body composition because it doesn’t differentiate between muscle and fat. Thus, an individual with a large amount of muscle mass could inappropriately be labeled as “overweight” or “obese” despite low levels of body fat. Conversely, individuals with low muscle mass and relatively high body fat may be classified as “normal”.
- Rather than assessing the lipid components that are directly linked to cardiovascular disease, Triglycerides and HDL-cholesterol, an optimal rating requires that the ratio of Total Cholesterol (TC) to HDL-cholesterol be less than 3.5:1. Contrary to conventional teachings, total cholesterol is not associated with increased cardiovascular risk. This old-fashioned mantra relies too heavily on the short-sighted assumption that LDL is the so-called “bad” cholesterol. Instead, the Triglyceride:HDL ratio appears to be the most reliable predictor of premature cardiovascular disease.
- Optimal health required the absence of a history of cardiovascular disease (CVD). This measure relied on self-reporting of prior events (heart disease, stroke, heart failure, etc.) and the use of a questionnaire to assess the presence of angina.
These points don’t necessarily invalidate the study. Rather, it’s important to understand the limitations of each measurement and the potential impact that each one has on the results.
The Findings
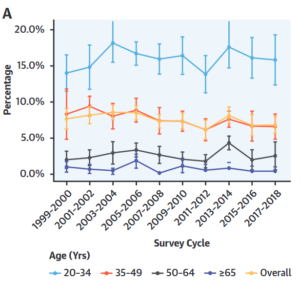
Optimal cardiometabolic health was defined as meeting the optimal criteria for each of the 5 metrics – adiposity, blood pressure, blood glucose, blood lipids, and absence of prior cardiovascular events.
Using these criteria, only 6.8% of adults had optimal cardiometabolic health.
For individuals over the age of 65 years, only 0.4% were considered to have optimal health. Even in the 20–34-year age range, only 17% of individuals have optimal health. Regarding differences by sex, only 3.1% of men and 10.4% of women were classified as optimal.
There was little difference in cardiometabolic health by income, but adults with lower education were half as likely to have optimum health as those with higher education.
The Takeaway
While I take issue with some of the metrics used to classify metabolic health, the overall message of the study is undeniably concerning. The metabolic health of our nation is alarmingly bad, and there has been a steady trend toward worsening over the past several years.
The data in this study are consistent with the data in the 2016 study, thereby giving us a clear picture of the poor metabolic health of our country.
At what point are we willing to admit that our public health messaging is ineffective or, worse, wrong? Perhaps we need to overhaul the Dietary Guidelines, which have been demonstrated to be unsupported by scientific evidence.
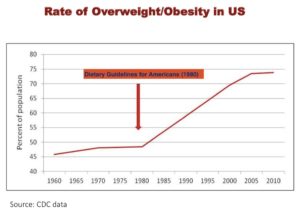
Regardless, given the absolute failure of our health “experts” to guide us effectively, it’s imperative that individuals be proactive about their own metabolic health.





