How to Optimize Your Health with a CGM
Glucose monitoring  has come a long way from when it was first recognized as a useful tool for managing diabetes. The use of Continuous Glucose Monitors (CGM) has revolutionized diabetes care by its ease of use and real-time data. They are gaining ground on conventional Fingerstick Glucose Meters as a more convenient method of glucose monitoring.
has come a long way from when it was first recognized as a useful tool for managing diabetes. The use of Continuous Glucose Monitors (CGM) has revolutionized diabetes care by its ease of use and real-time data. They are gaining ground on conventional Fingerstick Glucose Meters as a more convenient method of glucose monitoring.
What is a Continuous Glucose Monitor (CGM)?
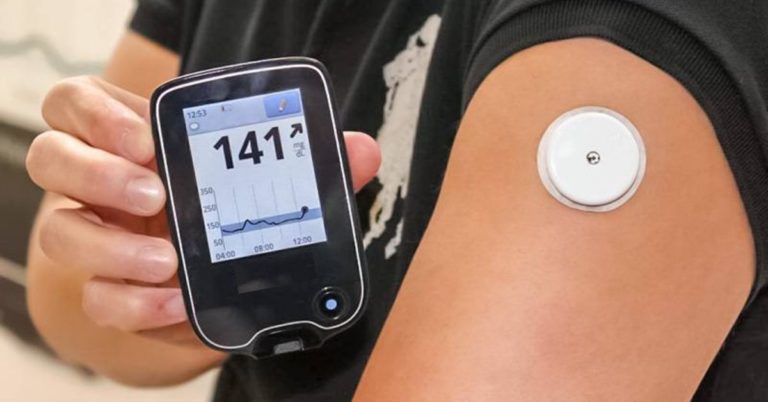
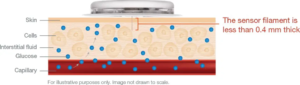
A CGM is an electronic device that is affixed to one’s body with a tiny plastic filament embedded in the skin that senses glucose levels. They communicate glucose data to an electronic device, most often via a smartphone app.
Continuous Glucose Meter vs Fingerstick Glucose Meter
Fingerstick glucose meters
The standard method of monitoring glucose has long been and still is the use of intermittent measurement by blood samples obtained by fingerstick. This method requires using a lancet to puncture the skin of one of your fingertips in order to produce a small drop of blood, which is then applied to a test strip that is inserted in the glucometer reading device.
Advantages |
Disadvantages |
| Option to test only as often as desired | Must carry multiple pieces – meter, lancet, test strips |
| Readily available technology | Glucose measurement is a snapshot in time – does not show glucose trend |
| Relatively cheap options available | Fingersticks may be painful |
Continuous Glucose Monitor (CGM)
Just as the name implies, it provides a continuous record of one’s glucose, thereby giving one a real-time look at your glucose levels rather than only intermittent snapshots.
Advantages |
Disadvantages |
| Ability to observe trends in glucose – may allow one to predict lows or highs before they happen | Expensive |
| Real-time, continuous data | Not a good choice for spot-checking glucose – by default, you get the continuous readings |
| Inconspicuous device attached to body | Each device typically lasts only 14 days |
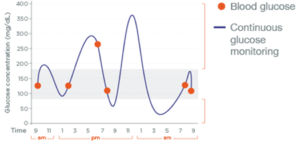
Because glucose meters give only a snapshot of the glucose level in the instant of when the blood specimen was obtained, standard glucose monitoring doesn’t show the whole picture of what your glucose trends are. In contrast, the CGM shows the entirety of data, thereby allowing you to see the ups and downs over time.
CGM use in diabetes
There are multiple studies demonstrating improved control of diabetes in individuals using CGM’s compared to the standard intermittent fingerstick testing.
CGM’s are especially valuable in individuals who are using insulin, as the continuous real-time data allows for more intensive monitoring and some devices even alert the user to abnormally low or high glucoses. Note that there is an inevitable delay in glucose values (several minutes) when measuring the interstitial fluid compared to blood glucose.
There is extensive data on the benefits of CGM’s in the management of diabetes, as well as improving length of stay (LOS) and outcomes in hospitalized patients1.
Also, there is a study in progress to assess whether CGM’s improve outcomes in Gestational Diabetes.
Because of their convenience and the availability of real-time data, CGM’s have also had a positive impact on quality of life for individuals with diabetes, contributing to overall well-being, less stress, less risk of hypoglycemia, better sleep, and better glucose control.
Are CGM’s useful outside of diabetes?
The astute researcher may note that there are no rigorous research studies (Randomized Controlled Trials) looking at outcomes related to CGM use in non-diabetics. That said, there is evidence that the optimal average glucose level is considerably lower than the threshold for diagnosing diabetes and that the risk of cardiovascular disease increases even below the threshold for pre-diabetes.
That should alarm you.
Said in another way: Even an average glucose level that is considered “normal” may put you at risk for cardiovascular disease.
It’s important to recognize that glucose tolerance (i.e. insulin resistance) exists on a continuum. The criteria for diagnosing diabetes and pre-diabetes are a human construct and are somewhat arbitrary, based on our best guess of when a high glucose is considered a disease state.
As referenced earlier, the use of a CGM can improve glycemic control in individuals with diabetes. Similarly, a CGM could assist individuals with managing their glucose tolerance such that they can avoid progressing to diabetes.
It’s short-sighted to say that a CGM should be used only by individuals with diabetes. Anyone with insulin resistance is likely to benefit from the use of a CGM by giving them insight into their glucose tolerance and the effects of their daily behaviors.
Granted, there may be decreasing marginal returns for healthier, more insulin-sensitive individuals, but considering that 93% of adults in the United States have poor cardiometabolic health, imagine the potential benefit of more widespread CGM use.
Blood sugar goals
There is reasonable evidence to support the following goals:
- Lower average glucose is better
- Lower glycemic variability (difference between highs and lows) is better
- Minimal glucose spikes
CGM use to optimize health
The Continuous Glucose Monitor can give you abundant, real-time glucose data. The following are various principles for using this data to improve various aspects of your metabolic health.
Evaluate the impact of food intake, as well as medications, supplements, etc.
See how these factors affect YOU, rather than just trusting what someone else tells you will happen.
- Assist with weight loss by eating foods that have less impact on your glucose
- Determine if order of food consumption has an impact on glucose
Evaluate the impact of activities, sleep, stress
- Determine optimal timing and amount of physical activity post-meal
- Determine optimal duration of sleep – sleep deprivation tends to increase glucose
- Increase motivation for physical activity.
Monitor glucose variability.
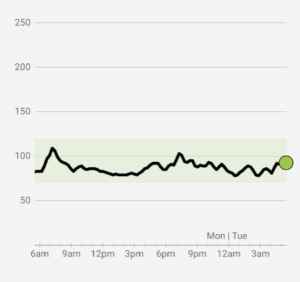
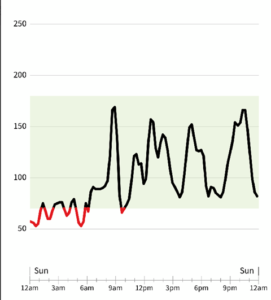
CGM’s are the most effective method for measuring Glucose Variability, the difference between the highest and lowest glucose levels. Aim for a relatively flat line; avoid peaks and valleys.
- Reduce hunger by decreasing glucose excursions – spikes cause damage, drops cause hunger
- Improve mood – high glucose variability associated with decreased mood
Reduce glucose spikes.
- An early sign of insulin resistance/prediabetes is significant post-prandial glucose spikes. Rapid return to baseline is a favorable sign.
Use CGM as an accountability tool and for motivation
- Use the real-time data to recognize the effects of your behaviors on your glucose levels
Other tips for using CGMs
- Start by using the CGM as a learning tool
- Take notes
- Expect a lag in glucose values – difference between blood and interstitial fluid
- Look at trends
- Test & re-test
- Avoid jarring the sensor – it may fall off and become unusable
- If you are getting low readings, cross-check with a fingerstick meter. Also, it appears that applying pressure to the sensor (such as lying on the sensor arm) may cause falsely low readings.
- Consider CGM data as one of many tools available to you, not the only measure that matters.