Mental Health – Part 3: A Closer Look at Treatments for Depression
Depression is one of the most common mental health disorders in the world and a leading cause of disability. It is a complex problem that has spawned a lot of research and a lot of theories about mechanisms of disease. In 1978, the American Psychiatric Association stated: “Psychiatric disorders result from the complex interaction of physical, psycho-logical, and social factors and treatment may be directed toward any or all three of these areas.” This statement is the closest thing we have to an official statement on the causes of psychiatric disorders.
In order to understand the approach to mental health disorders, let’s now examine more closely the current treatment options for depression as well as the potential for approaching depression as a neurometabolic disease.
Medications
Medications are the predominant form of treatment for depression, dominated by Selective Serotonin Reuptake Inhibitors (SSRIs) since fluoxetine (Prozac) was approved by the FDA in 1987, later sharing the market with other SSRIs including Celexa, Zoloft, Paxil, and Lexapro. There are other classes of antidepressant medications that have mostly fallen out of favor. SSRIs remain as the first-line treatment for depression, as well as for anxiety disorders.
Do SSRI medications work?
Prozac and multiple other medications in the same class were marketed under the premise that low serotonin levels were associated with depression and that the SSRI’s worked for depression by increasing serotonin levels. Subsequent research, however, h as concluded that there is no evidence of an association between serotonin levels and depression. That’s awkward. Especially when considering that Big Pharma has made a killing on antidepressant drugs, with a global market value in 2020 of $15.6 billion ($15,600,000,000).
as concluded that there is no evidence of an association between serotonin levels and depression. That’s awkward. Especially when considering that Big Pharma has made a killing on antidepressant drugs, with a global market value in 2020 of $15.6 billion ($15,600,000,000).
Also, it’s important to note that, in addition to many side effects from the medication, there is a significant (and miserable) withdrawal syndrome associated with abrupt discontinuation of SSRIs, something that I saw frequently in my hospitalized patients. For some individuals, it takes years to safely wean off the medications.
The Placebo Effect
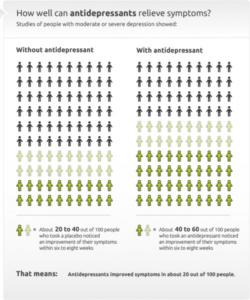
In a review of data submitted to the FDA to assess how effective medications are at treating depression, it was noted that approximately 82% of the response to antidepressant medication was duplicated in placebo control groups, meaning that the placebo effect appears to explain the majority of the benefit seen with treatment. In fact, only 43% of the trials submitted to the FDA showed a statistically significant benefit of drug over placebo.
How did the drugs get approved then? It turns out that only 2 clinical trials with significant benefit of drug over placebo are necessary to get FDA approval, no matter how many other trials there are that show no benefit. Any trial that doesn’t show benefit just gets ignored.
Are serotonin levels relevant?
Does serotonin really play a role in depression? A medication that actually causes decreased serotonin levels, tianeptine, was approved in France for treatment of depression. If the theory of increased serotonin levels helping in depression were correct, then patients on this medication should get worse. Instead, the clinical trials comparing this medication to SSRIs and tricyclic antidepressants showed that 63% of patients demonstrated improvement in their depression – the same response rate found for the other antidepressants. Thus, regardless of the effect on serotonin levels – increase, decrease, or no change – the medication simply doesn’t matter.
Therapy
Therapy remains an integral part of the management of depression, though unfortunately being utilized less and less over time despite being at least as effective as medication. In contrast to medication which can be effective only as long as it’s being taken, therapy has the potential to provide both immediate benefit and long-term benefit by preventing future episodes of depression.
Exercise
Exercise has been recognized as a beneficial intervention in depression, regarded as effective as an antidepressant medication. Exercise appears to be effective at reducing depression and may reduce relapse, but is underutilized.
It is also evident that physical inactivity is associated with symptoms of depression and anxiety
A Cochrane review showed that exercise contributes to moderate improvement in depression, but these results did not appear statistically significant when all examined studies were pooled together.
There were some noteworthy findings in this review, however, about specific forms of exercise. Resistance exercise showed a large benefit in depression, compared to only a modest benefit of aerobic exercise. Increased intensity of resistance training showed larger improvements than low intensity
Electroconvulsive Therapy (ECT)
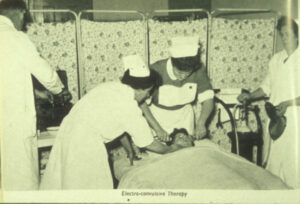 ECT has been around for 80+ years and yet remains one of the most controversial treatments in medicine. Essentially, it is the use of electricity to induce seizure activity. The mechanism is unclear, but it is superior to many other forms of treatment and has a clear anti-suicidal effect. Upwards of 80% of people treated with ECT respond favorably.
ECT has been around for 80+ years and yet remains one of the most controversial treatments in medicine. Essentially, it is the use of electricity to induce seizure activity. The mechanism is unclear, but it is superior to many other forms of treatment and has a clear anti-suicidal effect. Upwards of 80% of people treated with ECT respond favorably.
Transcranial Magnetic Stimulation (TMS)
TMS is a newer technique for depression that doesn’t respond to other treatments. It uses high-intensity magnetic impulses to stimulate the brain, potentially activating the brain networks that are underactive in depression. It has been used successfully in varying degrees in a number of brain conditions, including seizures, autism spectrum disorder, dementia, movement disorders, anxiety, and schizophrenia, while the evidence is best for its role in depression.
technique for depression that doesn’t respond to other treatments. It uses high-intensity magnetic impulses to stimulate the brain, potentially activating the brain networks that are underactive in depression. It has been used successfully in varying degrees in a number of brain conditions, including seizures, autism spectrum disorder, dementia, movement disorders, anxiety, and schizophrenia, while the evidence is best for its role in depression.
Nutrition
It can be difficult to assess the connection between depression and nutrition, as the depression itself may drive poor nutritional choices. The deficiency of several micronutrients is linked to depression and other mental health disorders, most commonly omega-3 fatty acids, B vitamins, minerals, and amino acids that are precursors to neurotransmitters. Accordingly, there is some evidence that high-dose supplementation of micronutrients improves multiple mental health disorders.
Changes in the dietary habits away from traditional diets are associated with chronic disease. For example, people living in the circumpolar region traditionally consumed nutrient-dense foods with high levels of protein, fat (especially omega-3 fatty acids), and antioxidants (e.g. selenium). Metabolic diseases like diabetes, obesity, and cardiovascular disease are historically rare in this population. As their dietary habits have transitioned to a Western-style diet that is high in carbohydrates and low in essential nutrients including omega-3 fatty acids, the population has also experienced rapid increases in said metabolic diseases. They have also historically had very low rates of mental health disorders, which have subsequently increased as their dietary habits have changed. There is consistent evidence that intake of omega-3 fatty acids and other nutrients inherent to traditional diets are beneficial for mental health.
away from traditional diets are associated with chronic disease. For example, people living in the circumpolar region traditionally consumed nutrient-dense foods with high levels of protein, fat (especially omega-3 fatty acids), and antioxidants (e.g. selenium). Metabolic diseases like diabetes, obesity, and cardiovascular disease are historically rare in this population. As their dietary habits have transitioned to a Western-style diet that is high in carbohydrates and low in essential nutrients including omega-3 fatty acids, the population has also experienced rapid increases in said metabolic diseases. They have also historically had very low rates of mental health disorders, which have subsequently increased as their dietary habits have changed. There is consistent evidence that intake of omega-3 fatty acids and other nutrients inherent to traditional diets are beneficial for mental health.
The first interventional trial to assess a dietary approach as treatment for depression was the SMILES trial, involving 67 individuals with depression who were consuming a “poor” quality diet. The intervention group was instructed to consume a Mediterranean-style diet focused on whole grains, vegetables, legumes, low-fat dairy, nuts, fish, lean red meats, chicken, eggs, and olive oil, while restricting sweets, refined cereals, and other processed foods. In a 3-month period, there was significantly greater improvement in depressive symptoms in the intervention group, one-third of whom met criteria for remission of their depression, compared to only 8% of the control group.
This study shows promise for the notion that diet is important for mental health. Eliminating processed foods, sugars, and refined carbohydrates appears to be important for mental health. There may be other dietary strategies that are even more beneficial but have yet to be examined in interventional trials.
Summary
Depression is a complex problem and among the most researched of mental health disorders.
It’s relatively safe to say that whenever there are multiple approved treatments for a condition, none of them are particularly effective.
There is mounting evidence that nutritional interventions may be an effective treatment strategy, not only for depression but also for a wide range of mental health disorders.
While depression and other mental health conditions may arise due to numerous factors, one’s underlying metabolic health likely has significant impact on the brain’s resilience and propensity to these conditions.





