Why US Health Care Ranks Last Among Developed Nations, and What to do About it
The United States is heralded as a center for innovation in the health sciences, esteemed as the location of many major advances in medicine and continually attracting the top talent from around the world. Despite these accolades, the US is far under-performing among the developed nations in terms of quality of health care and outcomes.
Even with such poor outcomes, however, the cost of said health care is substantially higher than the other nations. Thus, while ranking high in innovation and access to new treatments, the US ranked next-to-last in financial sustainability.
How the US pays for health care
Health insurance arose from the World War II era as a job benefit that could attract workers and that was exempt from the wage controls put into place by President Roosevelt (FDR). As a consequence of this tax-exemption (taken out of paycheck with pre-tax dollars), most people do not pay for their health care directly and thus are insensitive to the cost and value of that care.
Individuals are mostly insulated from the cost of their health care, because their insurance pays for it. Furthermore, they don’t actually know what their employers are paying for their health insurance. Thus, they don’t value what they are receiving and do not guard their health care spending as they do with spending in other arenas.
Health care across developed nations
The Commonwealth Fund survey of health care performance across 11 developed nations was last completed in 2021. It is noted that each country has quite varied approaches to how they structure health care services, and this report serves as a tool to gain insight into the approaches that are associated with superior performance.
The report looks at the following domains:
Access to care – affordability and timeliness of care
- The US ranks last, scoring significantly lower than the next-lowest country, Switzerland. This measure reflects denials of claims by insurance and difficulty paying medical bills.
- In terms of ability to get same-day care or after-hours care, the US ranked #9
Care process – preventive care, safe care, coordinated care, and engagement and patient preferences
- The US ranked #2 in this measure, reflecting things such as rates of mammography screening, influenza vaccination, and lifestyle counseling.
- US adults, however, have the lowest rates of continuity with the same physician
Administrative efficiency – time and effort spent with paperwork and administrative issues
- The US ranks last, reflecting difficulty faced by physicians in obtaining coverage of treatments or medications by insurance companies.
- US adults also spend more time on paperwork related to medical bills and are more likely to visit an emergency department
Equity – comparison in performance for higher and lower income individuals
- The US again ranked last, with the largest disparities in care between income groups
Health care outcomes – outcomes that can be modified by health care
- The US ranked last overall on outcomes, with the lowest ranking on 9 of the 10 outcome measures.
- The rate of preventable mortality in the US (177 deaths per 100,000 population) is more than double that of the best-performing country – Switzerland (83 deaths per 100,000).
The top-performing countries are Norway, the Netherlands, and Australia. The US ranks last at #11. In fact, the US ranked last in all domains of performance except care process, on which it ranked #2.

Despite such poor performance on all but one measure, the spending on health care as a share of gross product has increased substantially more than the other countries.
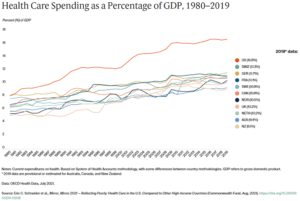
Comparing health outcomes to spending as a share of gross product shows how much the US is an outlier from the other developed nations.
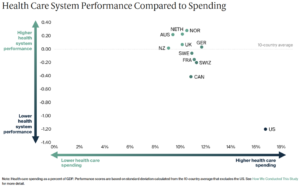
Common threads among high-performing nations
When comparing these developed nations on health care measures, what are the common features among the highest-performing countries?
- They provide for universal coverage and make health care affordable
- They invest in primary care to make health care accessible
- They reduce administrative burdens on both patients and clinicians
- They invest in social services that contribute to a healthier population and less demand on health care
Where the US struggles
It’s noted that the US is the only high-income country without universal health care. Many individuals in the US remain uninsured or under-insured, with potentially exorbitant out-of-pocket costs, as the insurance system is much to blame for the escalating cost of care in the US.
It is vital that efforts are made to improve access to high-quality primary care. US health care is largely focused on specialist care which results in expensive, siloed care.
In order to make health care more affordable in the US, there needs to be a reduction in the administrative burden placed upon clinicians. The rate of growth of administrators in health care is deplorable – there are too many talkers, not enough doers. That’s where your health care dollars are going.
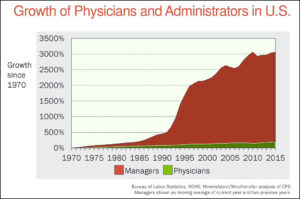
The solution
The solution to all of this nonsense is already available and is steadily growing throughout the US – it’s Direct Primary Care. It’s the only model of health care that has addressed the glaring deficiencies above that have plagued the US.
Direct Primary Care = High-quality primary care at an affordable price and accessible to all, free of administrative burden. That’s it…that’s all it takes to transform health care!
Direct Primary Care is the future of health care . . . and perhaps the only feasible way to make it sustainable.





