It’s Time to Set a Higher Bar for Health Care
When working in the hospital, I am often witness to the disappointingly low bar that has been set for metabolic health in our modern health care system.
One of my hospital patients was a gentleman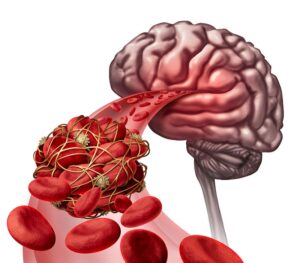 in his 7th decade of life who was admitted for a stroke (TIA – Transient Ischemic Attack, in his case). He sought medical care because he had sudden onset of difficulty with his speech along with some facial droop and decreased sensation on one side. Thankfully, his symptoms had resolved completely by the time I saw him the following day, and his neuroimaging (CT and MRI) showed no infarct (injury due to lack of blood flow). At that point, the role of hospitalization is to complete a workup to evaluate for potential causes of the stroke and to implement medical treatment aimed at preventing another event.
in his 7th decade of life who was admitted for a stroke (TIA – Transient Ischemic Attack, in his case). He sought medical care because he had sudden onset of difficulty with his speech along with some facial droop and decreased sensation on one side. Thankfully, his symptoms had resolved completely by the time I saw him the following day, and his neuroimaging (CT and MRI) showed no infarct (injury due to lack of blood flow). At that point, the role of hospitalization is to complete a workup to evaluate for potential causes of the stroke and to implement medical treatment aimed at preventing another event.
After addressing the acute issue of the stroke, I turned the discussion to his overall health. He takes 19 different medications, including:
- 3 medications including long-acting insulin, a GLP-1 agonist, and metformin for his type 2 diabetes,
- 4 medications for his blood pressure,
- 1 cholesterol medication (statin),
- 2 medications for anxiety/depression.
“How are your glucoses running at home?” I asked him, knowing that his Hemoglobin A1c is 7.8%, indicating that his average glucose for the past 3 months has been about 180 mg/dL (10 mmol/L). For reference, a normal Hemoglobin A1c is 5.6% or less, and a diagnosis of diabetes is established when the A1c is 6.5% or more. 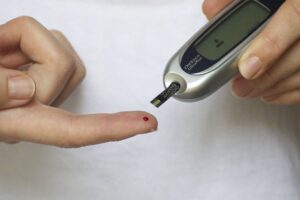
“Better recently”, he replied. He went on to say that his glucoses have been mostly below 200 and as low as 150.
“Hmmm…that’s not good,” I say.
“My doctor told me that 150 is good!” he retorted.
[My inner voice – CENSORED]
——————————————
Unfortunately, there’s nothing “good” about a glucose of 150. The proof is in the pudding — he’s lying in a hospital bed with a stroke!
[Let me make it clear also that this gentleman is not at all being faulted for this situation. In fact, I applaud him for sharing his perspective with me, and I explained to him why I’m so passionate about this issue. Rather, I am criticizing the medical community and health care as a whole for creating this culture of complacency about one’s most crucial asset — physical health.]
We’ve set a terribly low bar for health care, with doctors (and non-physician providers alike) accepting terrible glucose control as “normal”. The guidelines are not very stringent, suggesting a fasting glucose of 80-130 mg/dL and a post-meal glucose (90 to 120 minutes after a meal) less than 180 mg/dL in order to meet the A1c goal of 7.0%.
These values are far from normal, however. Normal fasting glucose should be 70-100 mg/dL, and post-meal glucoses should never exceed 140.
The consequences of this laxity with glucose control, however, are potentially catastrophic. Thankfully, this patient of mine did not suffer a devastating stroke, but we now know that he is at markedly increased risk for another vascular event going forward.
Cardiovascular disease is the leading cause of death in the United States, and it’s not slowing down. Diabetes is a significant risk factor for cardiovascular disease, and it’s important to realize that the risk starts well before a diagnosis of diabetes. In fact, the risk starts well before a diagnosis of prediabetes, even.
It’s time to set a higher bar for health care. With 93% of the country already suffering from poor cardiometabolic health, we can’t afford to continue accepting the current low standard.





